What is irritable bowel syndrome?
IBS is a health issue found in your intestines (gut). While the cause of IBS is unknown, it can still be treated.
IBS is a common health issue, impacting more than 35 million Americans. It does not cause lasting harm to the bowels and does not lead to intestinal bleeding or cancer.
There is no sign of disease when the colon is looked at and, much like a headache or muscle strain, IBS can cause a great deal of pain and distress, even though it cannot be seen.
IBS can cause symptoms such as:
- Belly pain.
- Cramping.
- Gas.
- Bloating (or swelling) of the belly.
- Change in stool.
There are different types of IBS, so each person may not have the same symptoms.
IBS-D: IBS with diarrhea
- You may often have loose stool.
- You may often feel an urgent need to move your bowels.
- You may often have cramps or belly pain.
IBS-C: IBS with constipation
- You may find it hard to move your bowels.
- You may not often move your bowels.
- You may have an urge to go but cannot go.
IBS-M: IBS mixed
- You may have symptoms of both IBS-D and IBS-C.
IBS can impact you physically, emotionally and socially.
Most people with IBS are able to control their symptoms through diet, stress management and, sometimes, medication prescribed by their doctors.
IBS results from a blend of many factors that can change how your GI tract works. Some factors that could cause IBS:
- Dysmotility — poor regulation of the muscle contractions of the GI tract causing abnormal movement.
- Visceral hypersensitivity — greater sensitivity of the nerves attached to the GI tract.
- Brain-gut dysfunction — problems in the connection between the nerves of the brain and gut.
Bowel movements: What is normal?
The frequency of bowel movements among healthy people varies from three movements a day to three a week, but each person has a different normal bowel function. A bowel movement each day is not needed for every person.
Stools should be formed but not hard, and they should have no blood. Stools should be passed without too much effort, straining or pain.
Terminology
Through the years, IBS has been called by many names — colitis, mucous colitis, spastic colon, spastic bowel and functional bowel disease. Most of these terms are not accurate. Colitis, for instance, means inflammation, or swelling, of the large intestine (colon).
IBS, however, does not cause inflammation and should not be confused with ulcerative colitis, which is a more serious health problem.
Note: IBS is not that same as inflammatory bowel disease (IBD). More information on IBD.
What are the symptoms of IBS?
Each person, based on the type of IBS they have, will have different symptoms. In general, IBS can cause:
- Belly pain.
- Cramping in the stomach area.
- Gas.
- Bloating (or swelling) of the belly.
- Diarrhea (loose stool).
- Constipation (hard stool or trouble passing stool).
- Urgent need to go.
- Sometimes, people with IBS pass mucus with their stool.
Each type of IBS can cause more specific, distinct symptoms.
IBS-D
- You may often have loose stool.
- You may often feel an urgent need to move your bowels.
- You may often have cramps or belly pain.
IBS-C
- You may find it hard to move your bowels.
- You may not often move your bowels.
- You may have urge to go but cannot go.
IBS-M: You may have symptoms of both IBS-D and IBS-C
Note: Bleeding, fever, weight loss and severe pain that does not go away are not symptoms of IBS and may suggest other problems. Talk to your doctor right away if you have these symptoms.
If you think you may have IBS — you have these symptoms more than three times a month for more than three months and it is getting in the way of your normal life — talk to your doctor. Speak up early, completely and often. Your doctor needs all the details of your symptoms to give you the best treatment plan.
Getting tested for IBS
To find out if you have IBS your doctor will do a few tests. Mainly, the tests will show whether you have a different health issue, such as an infection, causing your symptoms. There is no single test to make the diagnosis of IBS. If no other issue is found to be causing your symptoms, it is probably IBS, but only your doctor can confirm this.
Your doctor will:
- Ask you about details of your symptoms. Be prepared to be specific! Try a symptom tracker to help you stay organized.
- Do a physical exam, feeling your belly.
- Take your medical history to see if anyone in your family has other GI issues.
You doctor may:
- Do a blood test.
- Do a physical exam, feeling your belly.
- Do a stool test.
Based on the results of the blood or stool test, you may need other tests, such as a colonoscopy or endoscopy.
If other no other health issues are found, and you are having symptoms of IBS (such as cramps, belly pain, loose stool or problems passing stool) more than three times a month for the past three months, and it is interfering with your life, your doctor may conclude that you have IBS.
Treatments for IBS
There are many treatment options to help care for irritable bowel syndrome (IBS).
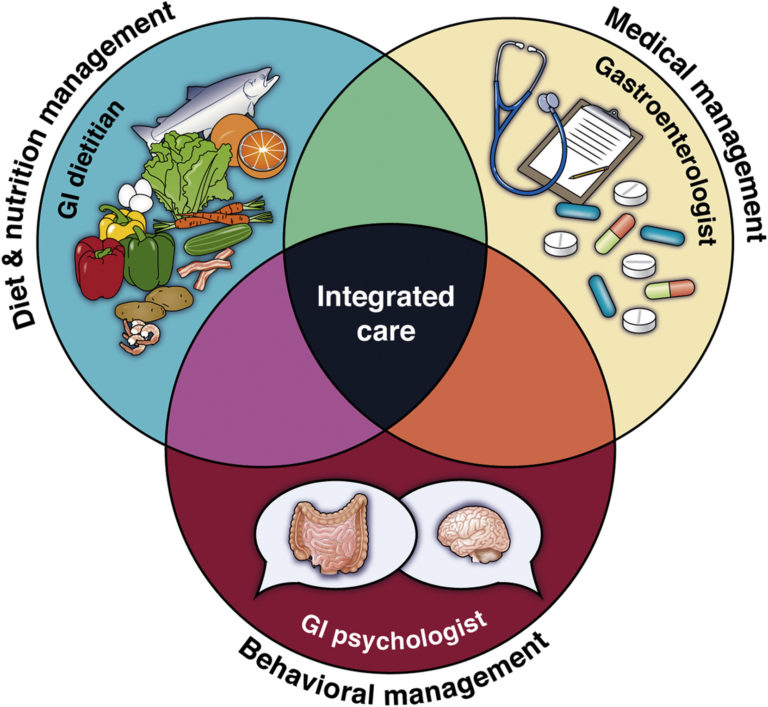
Talk to your doctor to find out which is best for you. Since each person experiences different symptoms with IBS, everyone needs a treatment plan unique to them. If you try one and are still having symptoms, let your doctor know so you can try something different.
Many people say that they feel their IBS symptoms after meals. For many people, eating a proper diet in small portions may help lessen IBS symptoms.
Before changing your diet, keep a record (food journal) noting which foods seem to cause what symptoms, and talk to your doctor about what you find.
Dairy products and high-fat foods often cause issues in some, but not all, IBS patients.
Recently, some IBS patients have lessened their symptoms with the low-FODMAP diet.
- FODMAP refers to a group of five sugars found in certain foods: lactose, fructose (in excess), fructans, galactans and polyols.
- Certain food items, if poorly absorbed, are broken down by bacteria to cause symptoms like gas, bloating or swelling, belly pain and loose stool.
Talk to your doctor or a registered dietitian before making any diet changes on your own.
IBS-D
- Over-the-counter or prescription drugs, such as loperamide, eluxadoline, rifaximin and alosetron, may be used to lessen or stop diarrhea (loose stool).
IBS-C
- Over-the-counter or prescription drugs (such as lubiprostone and linaclotide, which help pass stool), fiber supplements, stool softeners, laxatives and other medications that may stimulate motility (movement) or secretion of fluid in the intestines may be used to lessen or stop constipation.
Probiotics may also help IBS symptoms and are safe.
Sometimes, antibiotics can be used, but be careful not to use them too often.
Antidepressant and antispasm drugs can be used when stomach pain is really bad.
A number of new medications are in clinical trials, and hopefully, new treatments will be approved in the near future.
There are several psychological treatments that can help reduce the symptoms of IBS, including:
- Cognitive-behavioral treatment.
- Hypnosis.
- Stress management.
- Meditation
- Other relaxation methods.
These treatments seem to lessen stomach pain and the mental distress linked to IBS symptoms, improve coping skills and help patients adapt to their symptoms.
There are no harmful effects and these treatments can be used in addition to or instead of the usual medical treatments.
Talk to your doctor or health plan to put you in touch with a mental health professional to help you with these treatments.
Newly diagnosed
For some, finding out you have irritable bowel syndrome (IBS) is a relief, a reason for symptoms and a light at the end of the tunnel. For others, it can be scary and daunting. Many will have a mix of feelings. All of this is completely normal.
No matter what you may feel upon hearing you have IBS, it is of great value to know that you are not alone and that there are useful support groups for people with IBS (both in person and online) to deal with the impact on a physical, emotional and social level. If you are overwhelmed by your new diagnosis, don’t wait to reach out to a mental health expert to talk through the changes. He or she may suggest trying relaxation techniques, such as yoga, meditation or mindfulness.
Questions to ask your doctor
1. Will I need to do other tests in the future?
2. What if my treatment isn't working? How long should I wait to tell you if I am still having symptoms?
3. Are there symptoms that should cause worry? If so, what are they?
If you don’t know something at any point, ask for more (or clearer) information!
With your new IBS diagnosis, keep in mind:
- IBS can come in patterns, so figuring out your IBS pattern, what causes symptoms, when you feel at your worst and which medicines help and which don’t can help you and your doctor make a plan to live a normal, healthy life.
- Keep track of how you feel, what you eat, what stress you are feeling and what exercise you are getting.
- Certain foods like caffeine, fatty foods or alcohol can cause loose stools in many people but are more likely to impact those with IBS.
- Researchers have found that women with IBS may have more symptoms during their menstrual cycles (periods), so a female with IBS should try to prepare for symptoms around that time.
- Emotional worry (like travel or getting ready for a big speech) can cause symptoms of diarrhea (loose stool), constipation (hard stool or trouble passing stool) or pain in all people, but those with IBS can be more sensitive to these events.
Complications
IBS does not lead to more serious health issues, such as cancer or inflammatory bowel disease (IBD, ulcerative colitis or Crohn’s disease).
Some patients with IBS start feeling a lower quality of life due to symptoms such as pain, diarrhea (loose stool) or constipation (hard stool or trouble passing stool). This low quality of life could make you feel like not doing your normal routine. In these cases, your doctor may suggest working with a mental health professional.
Be sure to speak up early, completely and often. If you are having any symptoms, whether they are new or symptoms that won’t go away, tell your doctor.



